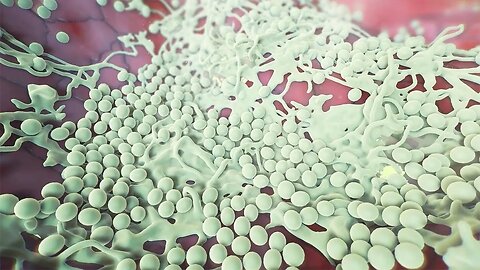
Treating and Preventing Vaginal Yeast Infections
MEDICAL ANIMATION TRANSCRIPT: A vaginal yeast infection is a common condition where too much yeast grows in a woman's vagina. Other names for it are vulvovaginal candidiasis and candida vulvovaginitis. Yeast is a type of fungus which is a plant-like organism. The type of yeast that usually causes the infection is called candida albicans. Your vagina is the passage from the uterus to the outside of your body. The surface inside your vagina normally contains small amounts of this yeast, which usually doesn't cause any problems. Other germs, such as the healthy bacterium Lactobacillus, also live in the vagina with Candida. They keep each other in balance. Sometimes conditions change in the vagina that make the yeast grow out of control. When this happens, yeast cells invade the lining of your vagina, called mucosal epithelium. As the yeast grows and damages your cells, it causes immune cells to enter the tissue. This inflames and damages the tissue as your immune cells try to clear the infection. Unfortunately, yeast cells can avoid immune destruction by killing immune cells. Or, yeast cells may grow too large for immune cells to destroy them. This allows the yeast to grow and spread, forming a layer called a biofilm in your vagina. It's not always clear why a person gets a yeast infection. But, you're more likely to get a yeast infection if you are pregnant, have diabetes. wash the inside of your vagina, also known as douching, have a weakened immune system, take birth control pills, or have taken antibiotics or steroid drugs. The most common symptom of a yeast infection is an extreme itchy feeling in your vagina and your vulva, which is the area around the entrance to your vagina. Other symptoms may include redness, burning and swelling in your vagina or vulva, pain during urination or sex, and a thick white odorless discharge from your vagina. You can treat a vaginal yeast infection with antifungal medicines. These medicines may be creams or suppositories that you apply in your vagina. Or, they may be pills you take by mouth. It's important to use an antifungal medication for as long as the directions tell you to. Don't stop using them early, even if your symptoms go away. Some of the ways you can help prevent a vaginal yeast infection include only washing your vulva, not inside your vagina, and not using douches or hygiene sprays. Keeping the genital area clean and dry. Not wearing tight underwear or pants. Wearing underwear with a cotton crotch. Always wiping front to back after using the toilet. Cleaning your vulva after sex. And, keeping your blood sugar under control if you have diabetes. Also, take antibiotics for other infections only as prescribed. Antibiotics may kill healthy bacteria that keep yeast in check, which can lead to a yeast infection. To find out more about vaginal yeast infections, talk to your healthcare practitioner.
#VaginalYeastInfection #VulvovaginalCandidiasis #CandidaVulvovaginitis
ANH23271
334
views
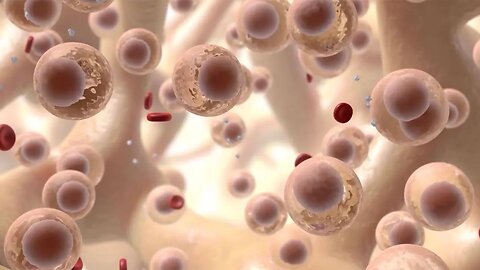
Managing Leukemia, Lymphoma, and Multiple Myeloma
MEDICAL ANIMATION TRANSCRIPT: You or someone you care about may have been diagnosed with a blood cancer. This video will help you understand how it can be managed. Blood cancer, also known as hematologic cancer begins in blood-forming tissues such as bone marrow. Bone marrow is the spongy tissue inside your bones that makes blood cells or blood cancer may start within the cells of the immune system. Examples of blood cancer are leukemia, lymphoma, and multiple myeloma. Treatments such as chemotherapy, radiation therapy, targeted therapy, immunotherapy, and stem cell transplant may control blood cancers depending on the type of cancer and other factors. It is important to have a care plan in place not only for receiving therapy and personal care but also for follow up care. This includes scheduling and going to follow-up appointments. In addition to checking your general health and wellbeing, your doctor will want to check for any signs of the cancer returning and check for health problems that may have resulted from treatment. For example, you may have tests and imaging studies performed, including taking samples of your blood, fluid around your spinal cord or bone marrow to check for cancer as relevant for your situation. Continue taking all your medications as prescribed. Do not stop taking them without talking to your doctor. It is helpful to take notes for points to discuss at your next doctor's visit. This could include any side effects you may have noticed. If you've had treatments such as chemotherapy, radiation therapy, or a bone marrow transplant, follow any instructions you were given. There are lifestyle changes that can improve your health and help you feel better. There are benefits to stopping smoking. This lowers the risk for cancer returning or spreading. It's generally accepted that eating a healthy diet can help you feel better and stronger both during and after treatment. Physical activities like walking, riding a bicycle or swimming can help you feel better and less tired. Talk to your doctor before starting an exercise routine. Knowing you have cancer can be overwhelming. You may have worries about your condition and how sick you could get, how it will affect you and your family, treatments and hospital stays, medical bills, and your job. There are ways to find support for you. Remember that your doctor and healthcare team are there to answer any questions you have. The following sources of support can help you, social workers, faith leaders, counselors, and support groups. Talk to your doctor if you have any questions about your treatment plan, medications or lifestyle changes to help you manage your blood cancer.
#BloodCancer #HematologicCancer #Leukemia
ANH19229
58
views
1
comment
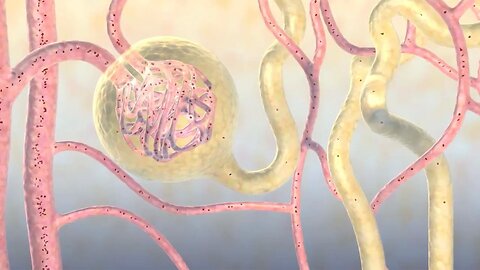
How Your Body Gets Rid of Medications
MEDICAL ANIMATION TRANSCRIPT: The body filters drugs from the bloodstream and eliminates them in a multi-step process called medication excretion. The kidneys are the major route for drug elimination. Most drugs exit the body either unchanged or as drug metabolites in urine. Generally, health professionals refer to the ability of the kidneys to filter blood as renal function. Nephrons, the functional and anatomical units of the kidney, filter blood, regulate fluid volume and pH, and control levels of electrolytes in the body. Each nephron contains a renal corpuscle and renal tubule. The renal corpuscle includes the Bowman capsule and glomerulus. And the renal tubule is composed of the proximal tubule, loop of Henle, distal tubule, and collecting duct. Each component plays a role in renal drug excretion, a four-step process that allows the kidneys to filter and eliminate drugs from the body. These steps are: glomerular filtration, passive tubular reabsorption, active tubular secretion, and excretion. Blood flows into the glomerulus via a blood vessel larger in diameter than the vessel draining blood from the glomerulus. This difference in diameter creates the high blood pressure necessary to filter wastes from the blood. The glomerulus functions as a molecular sieve. Waste materials in water pass through the sieve, while most normal proteins and cells are kept in the bloodstream. Glomerular filtration removes low-molecular-weight drugs from the bloodstream. The process of passive reabsorption of water, solutes, and ions begins in the proximal tubule, continues in the Henle loop, and ends in the distal and collecting ducts. Water-soluble drugs stay in the tubule, while unionized and lipid-soluble drugs are primarily reabsorbed across renal tubules. After reabsorption, lipid-soluble drugs travel through the bloodstream to the liver where certain liver enzymes, such as the cytochrome P450 enzyme complex, metabolize them into more water-soluble forms. Here we show an example of this process through the metabolism of pentobarbital. Some drugs are not filtered from the blood via the glomerulus. Instead, special anionic and cationic pumps in the walls of the renal tubule actively transport the drugs from the blood into the tubules and collecting duct. Urine from the collecting ducts travel through the ureters where it is collected and stored in the urinary bladder until elimination from the body. Although the kidneys are the major route for drug elimination, medication excretion can also occur in lactating women through their breast milk, exhalation through the lungs, release into bile, and elimination through saliva and sweat.
#MedicationExcretion #DrugElimination #kidneys
ANM10007
11
views
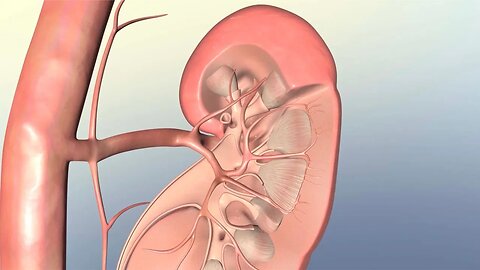
Understanding Kidney Failure
MEDICAL ANIMATION TRANSCRIPT: The kidneys are located on either side of the spinal column in the posterior abdominal cavity behind the peritoneum in the retroperitoneal space. The functions of each kidney include: filtration of metabolic wastes, fluids, and electrolytes from the blood during urine production, stimulation of red blood cell production, and regulation of blood pressure. The medullary pyramid and outer cortex compose the renal lobe, the structural unit of the kidney. Branches of the renal artery supply each renal lobe. The functional unit of the kidney is the nephron, composed of the renal corpuscle and the renal tubule. The renal corpuscle is where initial blood filtration occurs. It consists of a spherical network of capillaries called the glomerulus enclosed by a cup-shaped structure called Bowman's capsule. The size difference between the afferent arteriole and the efferent arteriole of the glomerulus creates the pressure that forces glomerular filtrate into Bowman's capsule. Reabsorption of water and other substances occurs in the renal tubule. Ninety-nine percent of the glomerular filtrate is reabsorbed as it passes through the parts of the renal tubule, including the proximal convoluted tubule, loop of Henle, distal convoluted tubule, and collecting duct. Acute renal failure is the sudden loss of the kidney's ability to remove waste and concentrate urine. Prerenal acute renal failure causes include anything that compromises blood flow to the kidneys such as hemorrhage or hypotension. Singularly or together, reduced blood pressure and reduced blood volume at the glomerulus result in less filtrate moving into Bowman's capsule. Intrarenal acute renal failure results from damage to nephrons. Toxins and lack of oxygen to kidney tissues can damage the nephron. Postrenal acute renal failure is associated with urinary tract obstructions such as kidney stones. Treatment for acute renal failure depends on the cause. Maintaining blood fluid volume, hemodialysis, or surgical removal of kidney tract obstructions may be required. Chronic renal failure is the loss of kidney function over a period of years. Nephron function is lost as a result of systemic diseases such as hypertension and diabetes mellitus, or kidney diseases such as chronic glomerulonephritis. Treatments include dietary control, including fluid restrictions, medication for the underlying condition, and electrolyte modifiers, ACE inhibitors for hypertension, and insulin therapy or hemodialysis can reduce chronic renal failure. End-stage renal failure usually requires dialysis and kidney transplantation. ♪ [music] ♪
#KidneyFailure #RenalFailure #kidneystone
ANM11017
25
views
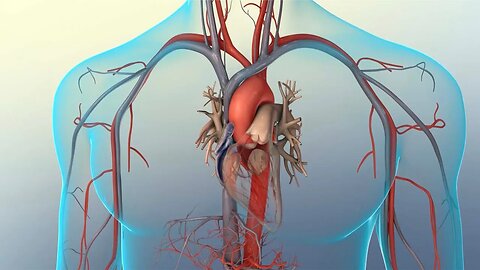
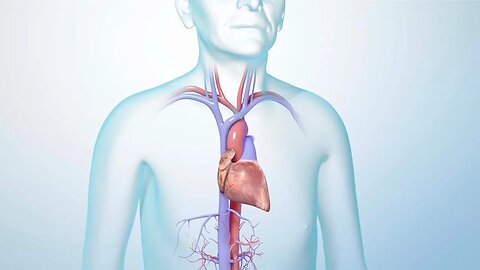
Understanding Your Heart Beat
MEDICAL ANIMATION TRANSCRIPT: The cardiac cycle is the sequence of contraction and relaxation of the heart chambers during a single heartbeat. The contraction of the heart chambers is called systole. And relaxation of the heart chambers is called diastole. The cycle begins with both the atria and ventricles in diastole. Both atrioventricular valves are open while the pulmonary and aortic semilunar valves are closed. Blood flows into the right atrium through the superior and inferior vena cava. Blood flows from the lungs into the left atrium through the pulmonary veins. Then blood moves from both atria into the ventricles through the open atrial ventricular valves. During atrial systole, the atria contract and force any remaining atrial blood into the ventricles. The ventricles are still in diastole, allowing them to expand and completely fill with blood. During ventricular systole, the ventricles contract, the atrioventricular valves close, preventing backflow or regurgitation of blood into the atria, the pulmonary semilunar valve opens, and the right ventricle expels blood into the pulmonary arteries to the lungs. Likewise, the aortic semilunar valve opens and the left ventricle expels blood into the aorta and out to the rest of the body. After ventricular systole, the cardiac cycle begins again as both the atria and ventricles enter diastole to allow the heart to fill with blood. Normally, this cycle repeats 60 to 100 times a minute. The right-side of the heart produces pulmonary circulation. This is the movement of deoxygenated blood from the body through the right atrium and ventricle, out through the pulmonary artery and to the lungs. Blood oxygenated in the lungs' alveoli returns to the heart through the pulmonary veins. The left side of the heart produces systemic circulation. This is the movement of oxygenated blood returning from the lungs to the left atrium and ventricle and out through the aorta to be distributed to the rest of the body.
#HeartBeat #CardiacCycle #BloodFlow
ANM11018
7
views
How to Manage Heart Failure
MEDICAL ANIMATION TRANSCRIPT: If you've been diagnosed with heart failure, it's important to control your symptoms. Heart failure, also called congestive heart failure, or CHF, is a lifelong condition in which your heart continues to work but not as well as it should. Your heart can't pump enough blood and oxygen to meet the needs of your body. Excess fluid builds up in the lungs, legs, and other body tissues. The symptoms of heart failure include shortness of breath, chronic coughing or wheezing, swelling of the legs, feet, or abdomen, weight gain, feeling tired all the time, nausea or lack of appetite, heart palpitations, difficulty lying flat due to feelings of suffocation, and having to sit up to breathe. Over time, heart failure weakens your heart and can shorten your life if not well managed. Fortunately, you can help control your symptoms by following your doctor's instructions, adopting a heart-healthy lifestyle, and staying aware of changes in your symptoms. Following the instructions of your healthcare team is very important in managing your symptoms and preventing unnecessary trips to the hospital. This includes taking your medications exactly as prescribed by your doctor. Don't stop taking your medications or skip doses. Take note of any side effects, and tell your doctor. If the cost of your medication is an issue, discuss other options with your doctor. Your medications may include angiotensin-converting enzyme inhibitors, angiotensin II receptor blockers, or angiotensin receptor-neprilysin inhibitors, beta-blockers, mineralocorticoid receptor antagonists, also known as aldosterone blockers, or sodium-glucose cotransporter 2 inhibitors. These medicines are important in managing heart failure. Don't take any over-the-counter medication or supplement without asking your doctor if it's okay. Make and keep all of your follow-up appointments for both doctor's visits and lab tests. Get vaccinated against the flu and pneumonia as directed by your doctor. Managing your heart failure also means adopting a healthy lifestyle. You may need to make the following changes. Eat a heart-healthy diet, including low-fat, low-cholesterol, and high-fiber foods. A heart-healthy diet helps you maintain or achieve a good blood pressure and weight and helps prevent other conditions that may further stress your heart. Check food labels for the amounts of these ingredients and others. Limit your salt and sodium intake to 2,000 milligrams a day, which is less than a teaspoon, by doing the following. Don't add salt when you cook or to food at the table. Avoid processed and fast foods. Compare food labels, and choose the items that are lower in salt and sodium. Limit your alcohol intake. Ask your doctor if your condition allows you to include any alcohol in your diet. Monitor your fluid intake. Too much fluid makes your heart work harder. Ask your doctor how much fluid is the right amount for you. Don't smoke. Nicotine increases heart rate and blood pressure. At the same time, it decreases the amount of oxygen-rich blood delivered to your body's tissues. Become physically active. Regular exercise through daily activities such as gardening and housework can make you feel better. Other good exercise options, with your doctor's approval, are walking, swimming, and bicycling. As you exercise, keep these precautions in mind. Rest as needed. Stop if you feel chest pain or more than usual shortness of breath. And don't exercise when temperatures are very hot or very cold. Your doctor may also prescribe a cardiac rehabilitation program that is a combination of medically supervised exercise, lifestyle counseling, and education. It is important to stay aware of changes in your symptoms and know when to get help. Using the traffic light colors, green, yellow, and red, to assess how you feel can help you take the proper action to manage your heart failure symptoms. Green is your goal and means that your symptoms are under control. Continue to follow your doctor's directions, and keep all medical appointments. Weigh yourself daily to see if your body is retaining fluids. Do it at the same time each day before eating or drinking, and wear the same type of clothing or no clothes at all. Record and take note of any changes in your weight. Symptoms in the yellow zone are warning signs. Call your doctor immediately if you gain 2 to 3 or more pounds in one day or 5 pounds in one week, have an increased shortness of breath, have difficulty sleeping due to trouble breathing, feel persistent, fast, or irregular heartbeats, or feeling lightheaded or as if you may faint. Red-zone symptoms are emergencies that mean you need medical evaluation right away. Call 911 if you experience chest pain that lasts more than 15 minutes, severe and ongoing shortness of breath, coughing up pink frothy foam, or fainting. Staying on top of your symptoms and following your doctor's instructions...
#HeartFailure #CongestiveHeartFailure #CHF
AND23020
81
views
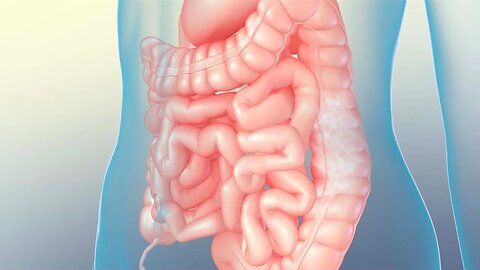
Understanding Lactose Intolerance
MEDICAL ANIMATION TRANSCRIPT: The digestive system consists of specialized organs and glands that process food and supply nutrients to body cells. The digestive organs form a continuous tube called the gastrointestinal tract. In normal digestion, swallowed food moves down the esophagus and into the stomach, where the food is broken down into smaller particles. From the stomach, these particles enter the small intestine, where enzymes from the pancreas, liver, and the intestinal lining breakdown the particles into nutrient molecules. Along the lining of the small intestine, cellular projections called microvilli absorb the nutrients as well as water, sugars, and fats. Unabsorbed food particles move into the large intestine which absorbs more water and salts. The remaining material enters the rectum, where it will stored until it exits the body as solid waste called feces. Lactose intolerance is an example of abnormal digestion. Lactose is the major carbohydrate in milk and milk products. Normally, ingestion of lactose stimulates cells lining the small intestine to secrete a digestive enzyme called lactase. Lactase divides the lactose into simple sugar molecules which are easily absorbed. In lactose intolerance, lactase is either absent or insufficient. After ingestion of food containing lactose, no lactase is available to break it down. As a result, lactose accumulates in the small intestine which disrupts normal water absorption, causing water retention. The unabsorbed water and undigested lactose enter the large intestine, where bacteria metabolize the lactose. This process generates gas that fills the large intestine, causing abdominal pain and flatulence. In addition, lactose in the large intestine causes water retention, producing watery feces known as diarrhea. While there is no cure for lactose intolerance, treatments include taking lactase tablets before eating foods containing lactose, using lactase enzyme drops in milk, and drinking lactose-free milk.
#LactoseIntolerance #lactase #FoodSensitivity
ANM11047
14
views
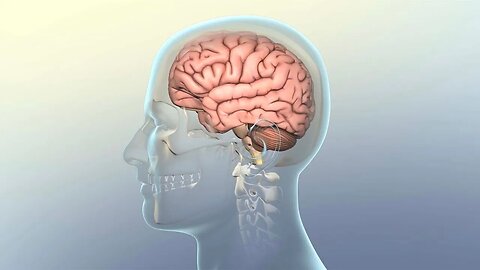
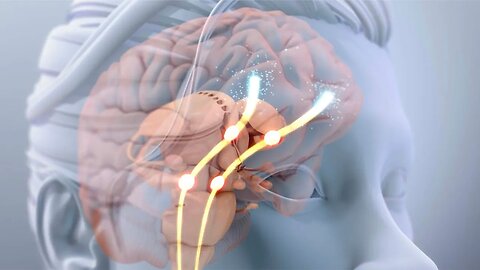
What is a Concussion and How Does it Affect The Brain?
MEDICAL ANIMATION TRANSCRIPT: A concussion is a brain injury resulting from a violent head impact or rapid head acceleration deceleration. The brain is a soft and pliable organ, and requires physical protection from the environment. The walls of the cranial cavity provide a hard external shield from outside impacts. Inside the cranium, the brain floats in and is surrounded by cerebrospinal fluid. Cerebrospinal fluid provides a protective cushion as everyday movements of the head gently jostle the brain. A violent impact or rapid acceleration deceleration of the head can cause the brain to rotate and strike the inside of the skull. This injury compresses the brain and sends shock waves rippling away from the point of impact. The impact force stretches or tears neuronal axons, resulting in a mild form of the traumatic brain injury called diffuse axonal shearing. This injury compromises normal brain function because it interrupts communication between neurons. Physical symptoms of concussion include headache, nausea, poor muscle coordination, dizziness, light sensitivity and blurred vision, ringing in the ears, and loss of consciousness. Cognitive and emotional symptoms include disorientation, confusion, amnesia, inability to focus and concentrate, irritability, and depression. Treatment for concussion depends on the severity and duration of symptoms. Mild concussions require plenty of rest, increased fluids, and close monitoring of symptoms for 24 to 48 hours. Although mild pain medication, such as acetaminophen or ibuprofen may be prescribed, alcohol and illegal drugs should be avoided. Severe concussions require immediate professional medical evaluation. In many cases, steroids are used to decrease swelling and inflammation in the brain. A CT scan or MRI of the brain may be needed to rule out gross internal damage or hemorrhages.
#concussion #BrainInjury #brain
ANM11014
26
views
What is Fentanyl and How Does it Treat Severe Pain?
MEDICAL ANIMATION TRANSCRIPT: Opioids are drugs that are prescribed to treat moderately severe or severe pain. Fentanyl is a strong synthetic opioid. It may be prescribed to treat severe pain from cancer or after surgery. Its potency, or strength, is up to fifty times that of heroin, an illegal opioid, and one hundred times that of morphine, another opioid used to treat severe pain. In order to understand how opioids like fentanyl work, it’s important to know how your body feels pain. The process begins when something harmful happens to your body. Information about this harm is converted to a nerve signal. The signal passes along nerves to your spinal cord and brain. In your brain, the signal is perceived as pain. Fentanyl affects how you feel pain. It attaches to structures, called opioid receptors. These receptors are found in cells in your brain, spinal cord, and other areas of your body. Fentanyl acts on these receptors to make you feel less pain. Fentanyl can also have other effects on your body. For example, it may give you an intense, short-term “high” and feelings of extreme happiness. Fentanyl also activates the reward pathway in your brain. This causes certain parts of the reward pathway to release a chemical, called dopamine. Scientists think dopamine helps you remember how good you felt while taking fentanyl, and makes you want to keep taking it. This link between remembering things that make you feel good with the desire to do them again is an important part of developing addiction. Fentanyl may also slow your breathing and make you feel nauseated. And, it may cause reduced motion of your intestines, resulting in constipation. There are two types of fentanyl: the pharmaceutical form, and the illicit, or illegal, form. While the pharmaceutical form of fentanyl may be prescribed to treat severe pain, it can be taken in ways that weren’t prescribed, such as taking too many, taking them to feel “high,” or giving them to someone else. The illicit form is made and sold illegally on the drug market. People take it because it produces a strong “high” and intense feelings of well-being. Fentanyl is a dangerous and addictive opioid because of its potency. As with any opioid, fentanyl addiction is a brain disease where you have an overwhelming craving for the drug. You can’t stop taking the drug despite the harm it may cause you. If you do stop taking the drug, you feel sick. This sickness is called withdrawal. Fentanyl withdrawal symptoms can be severe, which is why many people don’t stop taking it. Symptoms may include: anxiety, bone and muscle pain, increased heart rate, high blood pressure, vomiting and diarrhea, sweating and chills, and sleep problems. A fentanyl overdose means you’ve taken too much of the drug, which can cause life-threatening symptoms, or even death. Depending on your body size and how long you’ve been taking the drug, as little as two milligrams can kill you. Most cases of overdose and death from fentanyl in the United States are related to taking the illicit form. And, because fentanyl is strong and cheap to make illicitly, it’s often mixed with other illegal drugs, such as heroin, cocaine, and methamphetamines. This is dangerous because a person may take it without meaning to, which may result in accidental overdose or death. The symptoms of fentanyl overdose include: confusion; constricted, or “pinpoint” pupils; feeling sleepy or losing consciousness; weak, slowed, or stopped breathing; inability to talk; limp body; cold, clammy skin with discolored skin, lips, and nails; slowed or stopped heartbeat; and death. According to the Centers for Disease Control and Prevention, over one hundred and fifty Americans die each day from opioid overdoses, including fentanyl. If you have questions about fentanyl, or if you or someone close to you needs help for an opioid use disorder, talk to your healthcare practitioner.
#fentanyl #opioids #PainManagement
ANH23266
227
views
Nucleus Medical Media Celebrates 25 Years at SIGGRAPH 2023
Nucleus Medical Media celebrates twenty-five years of improving health literacy worldwide, with a retrospective look at how its medical animations have evolved over time to serve the education, healthcare, pharmaceutical, medical device, and biotechnology markets.
Nucleus was honored to have this animation accepted in the 2023 SiGGRAPH Conference’s Electronic Theater Retrospective Celebration that highlighted groundbreaking moments in computer graphics over the last 50 years.
#NucleusMedicalMedia #MedicalAnimation #siggraph
3
views